We're proud to announce Jenny Lange as a 2024 HDBuzz Prize winner! Our brains are made up of many types of cells that play different roles in the changes caused by HD. This study dives into a star-shaped cell called astrocytes and their role in HD.
Exciting new findings using 3D human lab-grown mini brains inform ongoing HTT-lowering trials and suggest that stem cell transplants for HD may improve cell-to-cell communication and reduce disease features.

Researchers with PTC Therapeutics recently published exciting new findings - a promising new huntingtin lowering drug that can be taken as a pill. Will this change how we move forward with huntingtin lowering?

Researchers show that highly expanded CAGs in the HD gene can cause early developmental changes using 3D brain models called organoids. What’d they find?
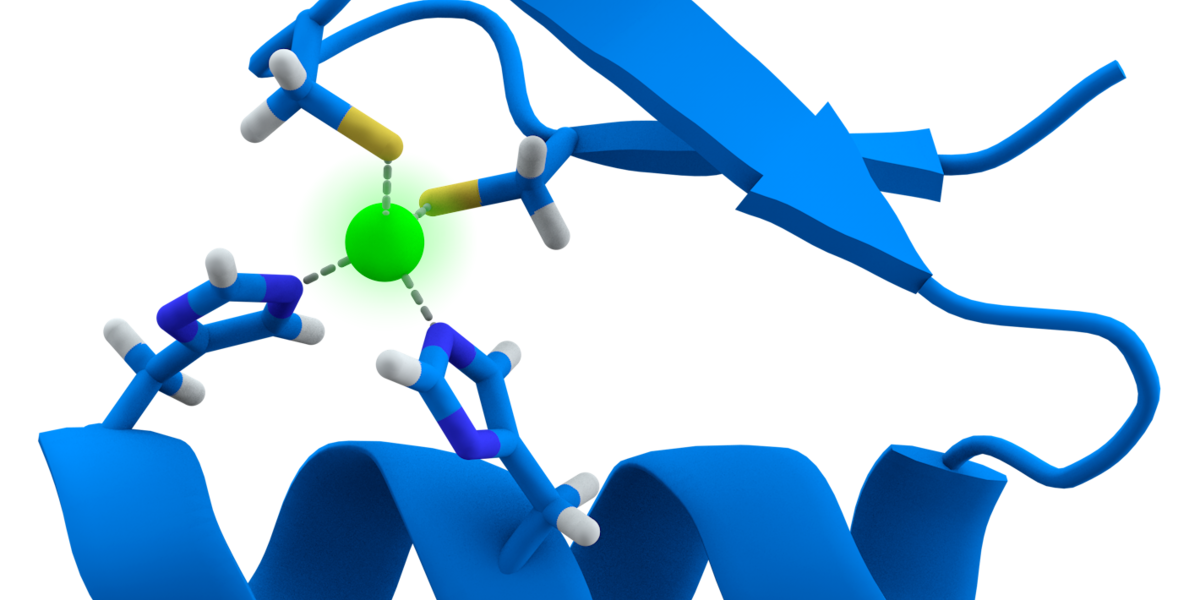
Exciting new Huntingtin Lowering work from @SangamoTx and @CHDIfoundation using "Zinc Fingers" to shut down expression of the mutant Huntingtin gene. More details on this exciting new technique here.
A surprising new paper sheds light on the role of the HD gene early in development. Should we worry?

Media reports of a wonder drug for neurodegenerative diseases like Huntington's disease are overhyped

Two recent studies show how a cellular border control system goes wrong in HD, opening new avenues for HD research.

Huntingtin helps fix damaged DNA, a recent study suggests, under the direction of a gene repair protein called ATM.