Exciting new findings using 3D human lab-grown mini brains inform ongoing HTT-lowering trials and suggest that stem cell transplants for HD may improve cell-to-cell communication and reduce disease features.

Our daily roundup of the science presented at the 2018 HD Therapeutics Conference in Palm Springs

HDBuzz summarises final day of the 2017 Huntington's Disease Therapeutics Conference in Malta
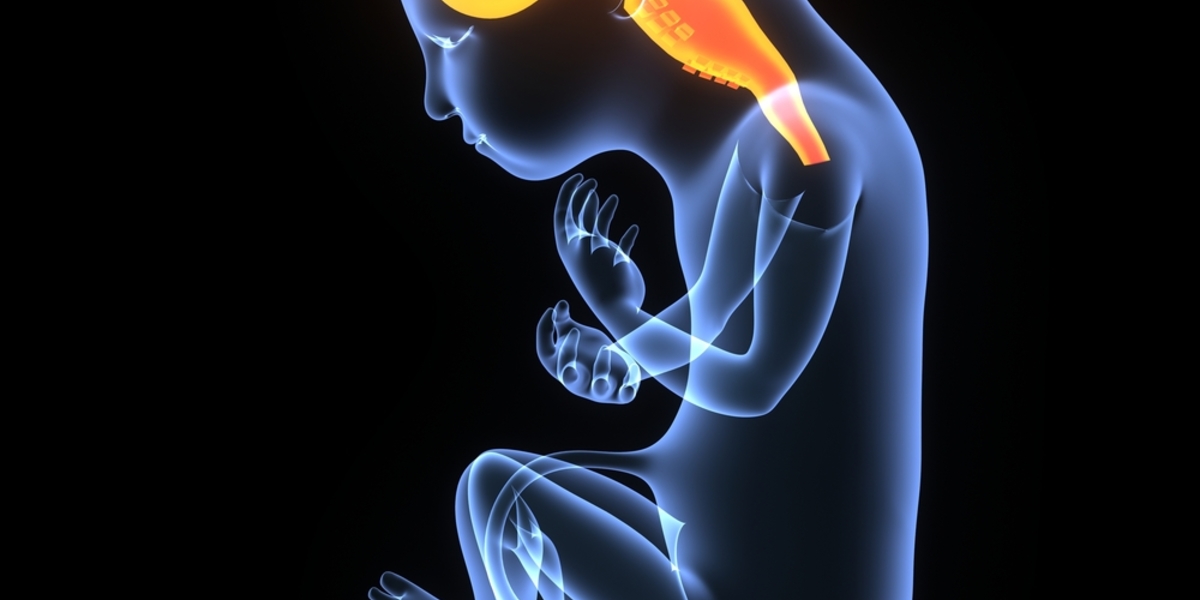
Is HD a developmental disease? HD stops neurons migrating in developing brain, but maybe we can get them going again
A new book for researchers describes a century of HD anatomy and presents evidence that HD affects the whole brain.
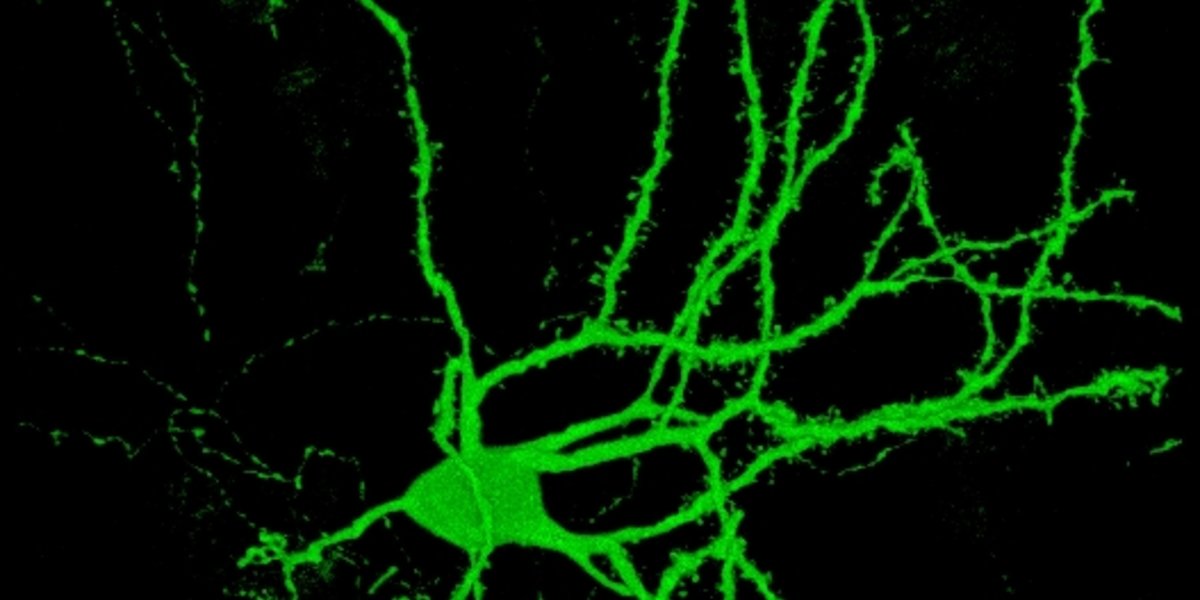
Scientists can now change human skin cells into working neurons, like the ones that are most affected in HD.
An important new study asks the question: what parts of the brain might need most help in HD?