
TRACK-HD reveals significant changes in pre-symptomatic HD mutation carriers and patients
The one-year report from the TRACK-HD study demonstrates a number of changes in pre-symptomatic HD-mutation carriers

TRACK-HD, an observational trial of people carrying the HD mutation has released data describing changes over the first year of the study. These data show that a number of changes can be robustly observed in a single year of observing HD patients, which could be used to help plan drug trials. Brain imaging, in particular, was able to clearly see changes caused by the HD mutation.
Drug trials and endpoints
All HD-affected people are hoping for successful drug trials that result in the discovery of effective treatments for HD. Discovering effective drugs is difficult, but the process of testing them is also complex. One of the difficulties for HD trials is knowing what to measure to decide whether the drug worked or not. It’s easy to imagine that a drug for cancer can be tested by measuring the size of tumors in patients who take the drug, compared with those that don’t. Tumor size, in this example, is what we call the endpoint of the trial, because it’s what actually gets measured. Drug trials succeed or fail based on these endpoint measurements.

Testing drugs for HD is a bit more complex than the cancer example. There are typical movements (chorea) that are associated with the disease, but they don’t occur until significant damage to the brain has already happened. Also, because we can identify people who will develop HD before they have symptoms by examining their DNA, we really want to treat people with drugs that delay the onset of HD while people are still well, rather than waiting for movement symptoms to occur. So we need to identify what changes occur early, and decide which of them are sensitive enough to use as endpoints in treatment trials.
TRACK-HD
The TRACK-HD trial, with sites in Canada, France, the Netherlands and the UK, aims to answer this question. Participants have a single visit every year for three years. The first, or ‘baseline’, visit for each patient occurred between January and August, 2008. The first follow up visits were between January-August, 2009. This trial is similar to the PREDICT-HD study, but is designed more like a drug trial. This means that it’s designed to be shorter (3 years), and only look for symptoms that change over this period. Because drug trials are very expensive to run, they will likely be of short duration, and in some ways TRACK-HD is like a ‘dry-run’ for these later studies.
The results of the first two assessments have just been published in the journal The Lancet Neurology.
Baseline differences and the need for longitudinal data
The baseline visit for TRACK-HD was conducted to look for differences between people carrying the HD mutation at different stages, and between those with the mutation and control subjects without it. Studies have already shown changes like this, so it was important for the TRACK-HD study to measure those effects in more detail. Also, because HD takes many years or decades to develop, differences seen in HD patients may seem large at the baseline but actually be due to very slow changes that take place over a long time. These kinds of differences would be bad endpoints for a drug trial, because the change in following years will be very small and difficult to measure. The TRACK-HD baseline data was published in 2009, and showed a number of important differences in HD mutation carriers and patients.
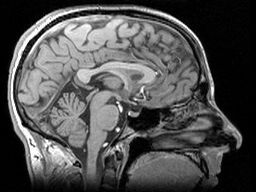
Categories of study: brain imaging, cognitive, motor and psychiatric
What are these ‘changes’? The TRACK-HD study is conducting a large number of measurements on each subject. Magnetic resonance imaging (MRI) captures a detailed three-dimensional picture of the brain of each subject. Motor (movement) symptoms are being measured in a number of ways, including high-tech eye movement tracking and other sophisticated tools. A number of tests are designed to test the intellectual (or ‘cognitive’) function of subjects, and their emotional wellbeing. Finally, there are a number of rating scales that have been used by physicians to score signs of HD, and these were measured as well, allowing the TRACK-HD scientists to compare their information to older trials. This is a lot of tests, and TRACK-HD participants should be congratulated for their contribution to the entire HD community.
Most sensitive measures
Having the baseline data for each subject let the scientists in TRACK-HD look at the change of each measurement over the first year. Of the dozens of measurements made, those derived from brain imaging were the most sensitive. Analyzing changes in hundreds of three-dimensional images is difficult, so TRACK-HD scientists used three completely distinct techniques to make sure changes they observed weren’t due to technical problems. The answers they received from each technique agreed with one another very well, giving us confidence that they’re measuring real changes in the brain.
The volume of the whole brain decreases faster in people carrying the HD mutation, although it also shrinks over a year in people without the HD mutation. Specific regions of the brain that are known to be very sensitive to HD called the caudate and putamen degenerated even faster in people carrying the HD mutation. The study also found early losses of the white matter of the brain, which is important stuff because it’s the ‘wiring’ of the brain.
Some tests of intellectual function were worse in HD mutation carriers, especially a circle-tracing test. This simple task required subjects to accurately trace a circle on a computer screen, which requires good fine control of movements. Performance on this task degenerated in nearly all groups of people carrying the HD mutation, including people some years from expected onset of symptoms. A number of other cognitive function tests used in HD trials didn’t change enough over the course of a year to be useful in a short drug trial in pre-symptomatic HD mutation carriers.
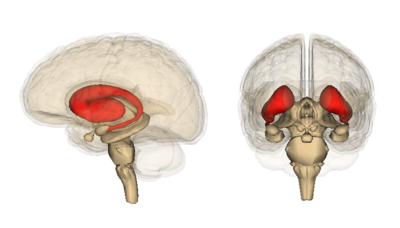
Image credit: Life Science Databases
Difficult emotional behavior, including irritibility and apathy, happened more frequently in HD mutation carriers at the baseline visit. But, according to the follow up study, these symptoms didn’t change very much in one year. These types of measurements may not be a good basis for a short-term drug trial. This is interesting, because it implies that some symptoms of HD, like irritibility and apathy, develop very slowly while other changes might be more sudden.
Power analysis and the future
Of the dozens of measurements for each TRACK-HD patient, the loss of tissue in the caudate region of the brain was the clearest change observed. This loss of tissue was consistently higher in every group of HD mutation carriers observed, even those years before expected motor symptoms of HD. This information allows the scientists running this study to suggest that measuring the volume of this brain region might be a good endpoint for a drug trial in HD.
What would a trial using this information look like? How many people would have to participate to ensure that the trial gave conclusive information? Using the observed changes, the TRACK-HD scientists can calculate how large a study would have to be, in order to give conclusive information. To do this, we have to estimate how effective our drug would be. If the drug slowed down the loss of caudate volume by 20%, we would require 354 patients to take drug, and 354 patients to take a placebo, or control substance. This number of patients give us enough information to determine whether the drug worked. A more potent drug that prevented 40% of caudate shrinkage would only require 89 patients to take drug and 89 patients to take placebo.
This is hopeful news, because the HD community has shown it can fill drug trials with these kinds of numbers. For example, an ongoing trial of coenzyme Q10 has 608 participants and CREST-E is testing creatine in 650 people. TRACK-HD provides hope that, if we can find the right drug, we will be able to successfully test it.
Learn more
Sources & References
For more information about our disclosure policy see our FAQ…


