COVID-19 update: what does it mean for HD families, how does it impact HD research, and how has it changed the way science works?

The news has recently been full of stories about CRISPR, a new "jaw-dropping" DNA-editing technology. Hype or hope?
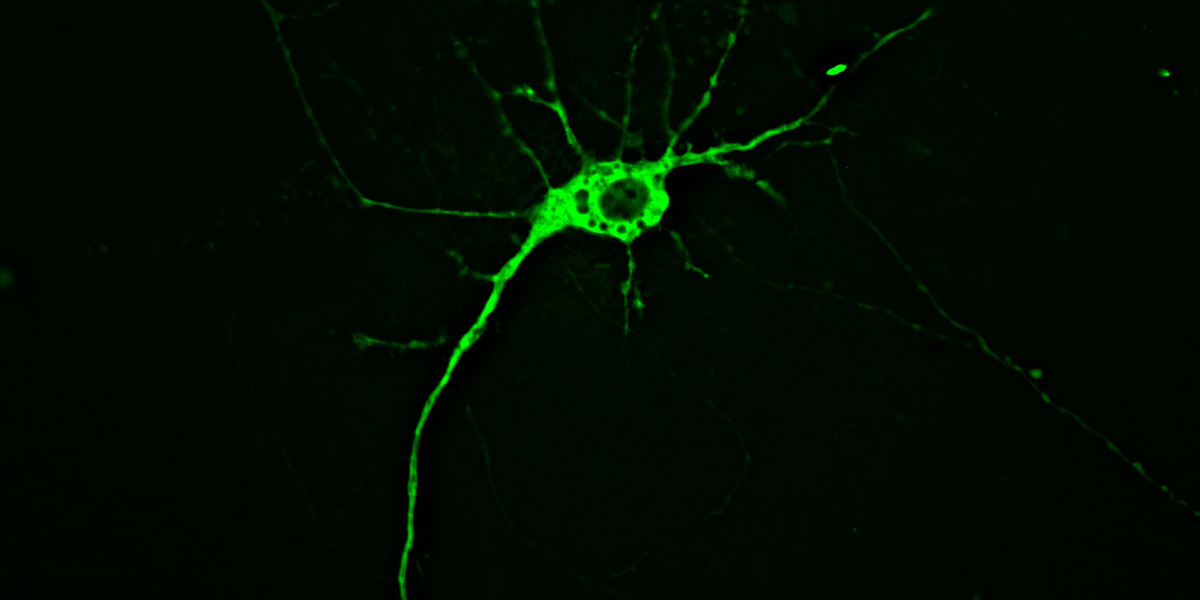
Researchers have used mice with glowing brain cells to decipher the first steps of neurodegeneration
A new antibody lets scientists identify neurons that are going to die after producing mutant huntingtin
Scientists use beams of neutrons to study the structure of clumps of mutant huntingtin protein

Advanced drug screening techniques help scientists to make drugs that increase cellular recycling in neurons.