Huntington's disease therapeutics conference 2019 – Day 2
New tools to bridge the gap between the lab and patients in our update from day 2 of the 2019 HD Therapeutics conference

Jeff and Ed report from the Huntington’s Disease Therapeutics Conference – the biggest annual gathering of HD researchers. This year’s conference is bigger and more exciting than ever.
Read about Day 1 here.
Advanced tools for translational research
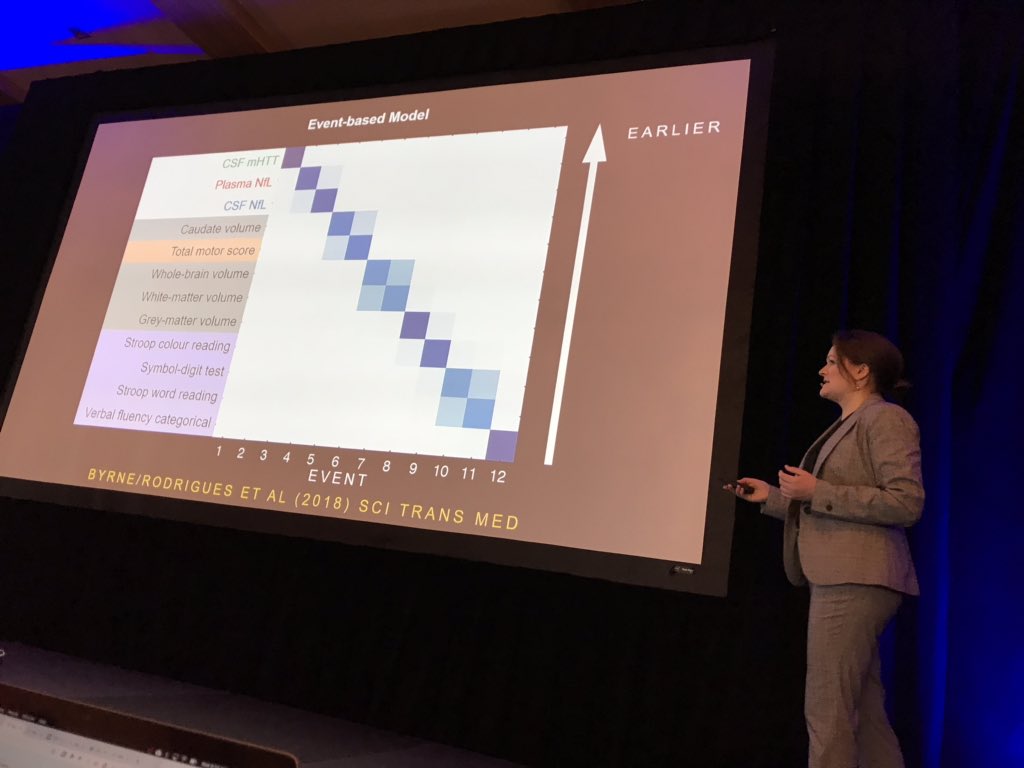
Morning everyone! The second day of the 2019 HD Therapeutics Conference is kicking off in Palm Springs. The first session is “advanced tools for translational research”.
The first speaker today is Lauren Byrne from UCL who studies biomarkers in blood and cerebrospinal fluid. Byrne measured mutant Huntingtin in CSF, and neurofilament light protein in CSF and blood in 80 volunteers. Neurofilament light or NFL is a protein found in neurons and released when they are damaged. Byrne also did MRI scans to see how each biomarker predicts brain shrinkage. Surprisingly, neurofilament turns out to be a better predictor the mHTT of clinical symptoms and brain volume. Changes in these “biofluid” markers were among the earliest detectable changes too, preceding imaging and clinical measures in the sequence of events in HD.
Byrne has now completed the 2-year follow ups from the HD-CSF study and shows that the NFL seems to be changing as expected over time, and can be measured using a new system that tests 4 molecules at once.
Next up is Amber Southwell, from UCF, who is also interested in developing tools to quantify mutant huntingtin in the spinal fluid. Southwell’s team was the first to show that when mice are treated with a Huntingtin lowering therapy – specifically an ASO from Ionis Pharma – levels of mutant Huntingtin in the spinal fluid are reduced. This is important – it means that when we treat human HD patients with Huntingtin lowering drugs, we’d predict that the levels of mutant Huntingtin in the spinal fluid will go down. This is one of the things reserarchers mean when they say a measurement is a “biomarker”.
Southwell’s team is doing a cool series of experiments with mice that have no Huntingtin in specific types of brain cells. This is enabling them to map the exact type of brain cell responsible for releasing mutant Huntingtin into the spinal fluid.They’re also conducing another set of experiments focused on understanding the exact process by which mutant Huntingtin makes its way from brain cells called neurons into the spinal fluid. One process of brain bathing called “glymphatic clearance” seems likely to play a role in mutant Huntingtin making it’s way into the spinal fluid.
Next is David Salzman of sRNAlytics, a company that investigates the use of RNA to study diseases.RNA is the single-stranded cousin of DNA. Cells use RNA for many functions, most famously as the “working copy” of genes they want to switch on. That’s called messenger RNA. Less famously, cells produce many small RNA molecules that help in the regulation of gene switching. They have names like microRNA and there are lots of different ones.We understand genes as recipes for proteins pretty well, but micro RNAs are much morel mysterious at the moment.

SRNAlytics identifies patterns of small RNA changes and uses artificial intelligence algorithms to identify what part of the body they come from, and how they change in different diseases. A panel of 60 small RNAs in CSF can apparently distinguish between Huntington’s, Alzheimer’s and Parkinson’s with decent accuracy. Two small RNAs are of particular interest in HD, but it’s important to understand exactly what they do in healthy and HD brains in order to figure out their value as possible biomarkers.
New animal models
Guoping Feng, from MIT, is up next. His lab is working on developing new primate models of HD. He says mice are very useful, but they don’t have all the same brain regions as humans, so we need to study more sophisticated brains as well. It used to be difficult to impossible to genetically modify primates, like monkeys, but new genome engineering tools make it possible. Tools like CRISPR/Cas9 allow precise DNA edits to be made to the DNA of monkey embryos. Feng’s lab is one of the world’s best at making changes to primate DNA. He describes that they’ve learned from human IVF clinics the best ways to keep primate embryos healthy. Feng’s lab has generated a novel monkey model of a genetic form of autism. These monkeys have very interesting behaviors that really resemble humans with Autism, including altered social behaviors. They are now working to develop a monkey model of Huntington’s Disease, and have conducted initial experiments suggesting it should be possible.
Hideyuki Okano, of Keio University, also works on primate models of human diseases – specifically Marmosets. His lab has genetically modified Marmosets to have a form of Parkinson’s Disease caused by a genetic mutation. These animals have symptoms very close to those observed in Parkinson’s Disease patients, including a very challenging sleep condition called REM sleep behavior disorder (RBD). They also have tremors and walking problems that resemble Parkinson’s Disease patients. It’s a good argument for using more more sophisticated animals to model progressive brain diseases. Okano’s lab is now developing techniques to generate similar models for Huntington’s Disease.
Thats all for today! Be sure to check out our write up of day 1 here and stand by for our final roundup tomorrow.
For more information about our disclosure policy see our FAQ…